Dic amniotic fluid embolism1/11/2024  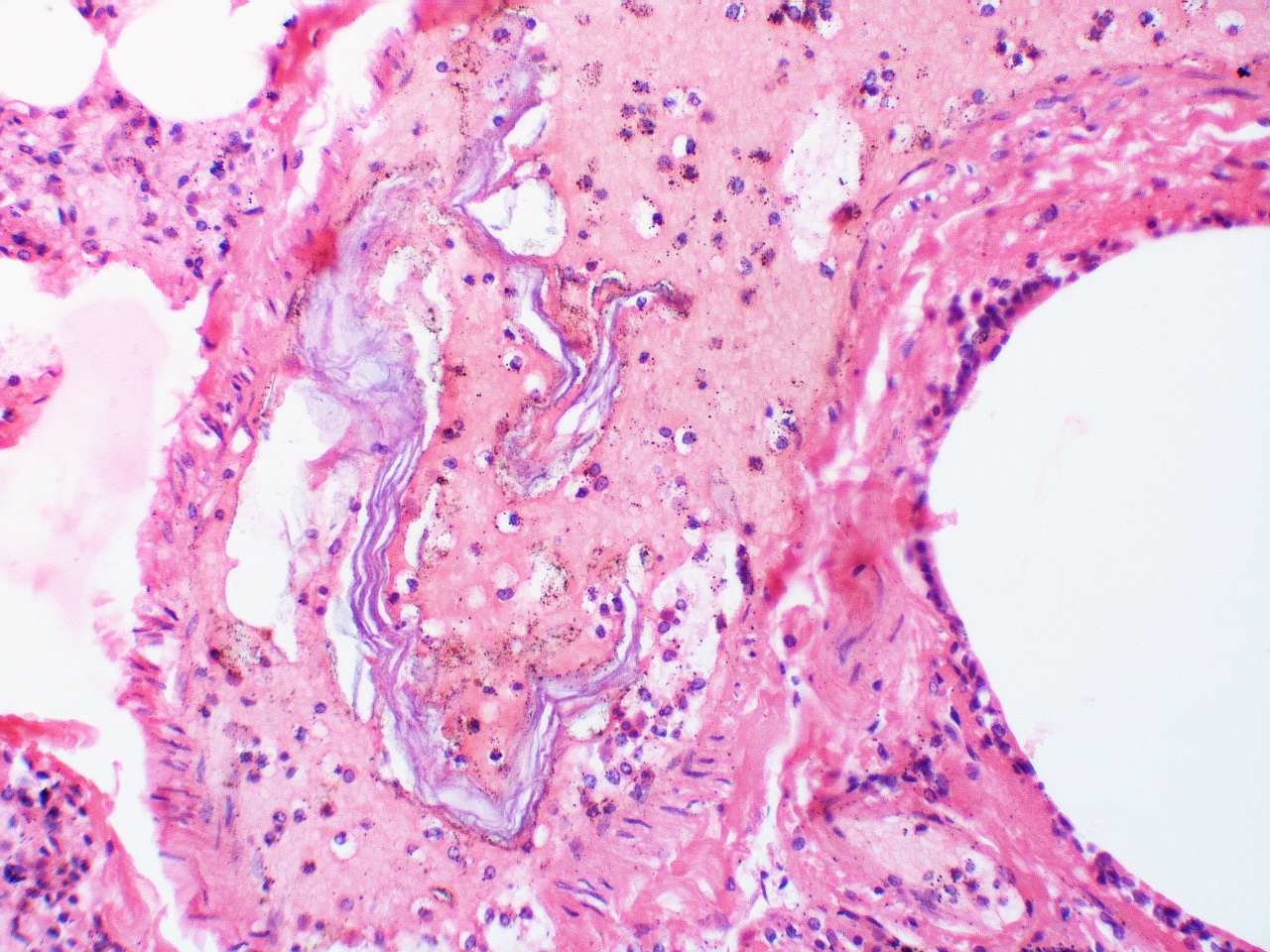
A hypothesis regarding complement activation and amniotic fluid embolism. The role of echocardiography in amniotic fluid embolism: a case series and review of the literature. Simard C, Yang S, Koolian M, Shear R, Rudski L, Lipes J. Incidence and risk factors of amniotic fluid embolisms: a population-based study on 3 million births in the United States. Amniotic fluid embolism: an evidence-based review. Amniotic fluid embolism: update and review. Pulmonary vascular obstruction by squamous cells is not involved in amniotic fluid embolism. 2014 123:337–48.įunk M, Damron A, Bandi V, Aagaard K, Szigeti R, Clark S. Amniotic fluid embolism: an Australian-New Zealand population-based study. Despite prior reports of mortality rates exceeding 80%, current evidence supports a mortality rate of approximately 20%. The diagnosis of amniotic fluid embolism is a clinical diagnosis of exclusion there is no gold-standard test or biomarker. Amniotic fluid embolism is thought to occur when amniotic fluid enters into the maternal systemic circulation through a breach in the maternal–fetal interface, leading to the release of inflammatory mediators and endogenous catecholamines that cause acute cor pulmonale and severe disseminated intravascular coagulation (DIC). Although rare in an absolute sense, amniotic fluid embolism is identified as the leading cause of maternal mortality in many developed countries. Amniotic fluid embolism is characterized by the sudden onset of hypotension, hypoxia, and coagulopathy during, or immediately after, delivery. Intensivists are often called upon to co-manage cases of suspected amniotic fluid embolism with our colleagues in obstetrics and anesthesia, so familiarity with this condition is essential. All rights reserved.Amniotic fluid embolism is one of the most devastating complications in obstetrics. In cases that require prolonged cardiopulmonary resuscitation or, after arrest, severe ventricular dysfunction refractory to medical management, consideration for venoarterial extracorporeal membrane oxygenation should be given.īlood product cardiac arrest coagulation cryoprecipitate dobutamine norepinephrine platelet right ventricular failure.Ĭopyright © 2019 Elsevier Inc. Amniotic fluid embolism-related coagulopathy should be managed with hemostatic resuscitation with the use of a 1:1:1 ratio of packed red cells, fresh frozen plasma, and platelets (with cryoprecipitate as needed to maintain a serum fibrinogen of >150-200 mg/dL). Blood pressure support with vasopressors is preferred over fluid infusion in the setting of severe right ventricular compromise. If such failure is identified, treatment that is tailored at improving right ventricular performance should be initiated with the use of inotropic agents and pulmonary vasodilators. Where available, we recommend performing transthoracic or transesophageal echocardiography as soon as possible because this is an easy and reliable method of identifying a failing right ventricle. We describe key features of initial treatment of patients with amniotic fluid embolism. Because amniotic fluid embolism usually is seen with cardiac arrest, the initial immediate response should be to provide high-quality cardiopulmonary resuscitation. Amniotic fluid embolism is an uncommon, but potentially lethal, complication of pregnancy. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
